Overview

Fallen arches, also know as having flat feet, or pes planus, refers to the collapsing of the foot?s arch so that it is no longer curved properly or adequately supportive. The condition can cause foot pain, fatigue and affect gait, which can create strain on the knees, ankles legs and hips. Fallen arches can occur naturally from birth, or can be attributed to the rolling in of the foot and ankle while running (overpronation).
Causes
Genetic predisposition. Faulty foot mechanics, e.g. excessive pronation. Abnormal bony architecture. Laxity of ligaments. Neuro-muscular disease. Trauma to the leg muscles or major tendons. Inflammatory diseases of the joints e.g. Rheumatoid arthritis. Surgical procedures on the leg and ankle. Limb length inequality. Tight Achilles tendon.
Symptoms
Flat feet can cause a myriad of symptoms, from experiencing pain in the foot, heels, arch, calves, the shin, the knee, the hip and into the lower back due to overworking of the hip flexors or they may find it hard to stand on tip toes.
Diagnosis
People who have flat feet without signs or symptoms that bother them do not generally have to see a doctor or podiatrist about them. However, if any of the following occur, you should see your GP or a podiatrist. The fallen arches (flat feet) have developed recently. You experience pain in your feet, ankles or lower limbs. Your unpleasant symptoms do not improve with supportive, well-fitted shoes. Either or both feet are becoming flatter. Your feet feel rigid (stiff). Your feet feel heavy and unwieldy. Most qualified health care professionals can diagnose flat feet just by watching the patient stand, walk and examining his/her feet. A doctor will also look at the patient's medical history. The feet will be observed from the front and back. The patient may be asked to stand on tip-toe while the doctor examines the shape and functioning of each foot. In some cases the physician may order an X-ray, CT (computed tomography) scan, or MRI (magnetic resonance imaging) scan.
What is PES Planovalgus deformity?
Non Surgical Treatment
If you have flat feet and foot pain, especially if one foot is flatter than the other, you should have an evaluation by an orthopedic surgeon . You may have a problem with the posterior tibial tendon , the main tendon that supports the arch. Factors that can contribute to this problem are obesity, diabetes , high blood pressure , certain types of arthritis and athletic overuse. In some cases a shoe insert/orthotic can be used to alleviate the symptoms of flat feet.
Surgical Treatment
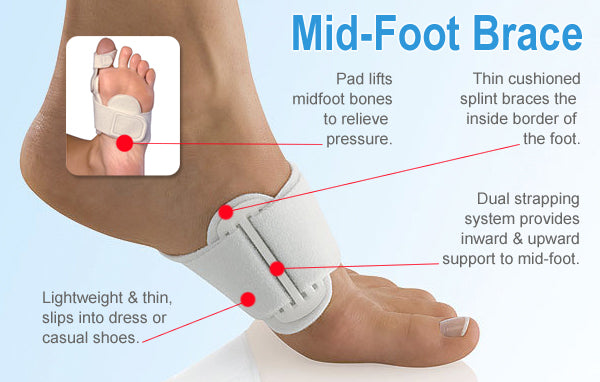
Rarely does the physician use surgery to correct a foot that is congenitally flat, which typically does not cause pain. If the patient has a fallen arch that is painful, though, the foot and ankle physicians at Midwest Orthopaedics at Rush may perform surgery to reconstruct the tendon and "lift up" the fallen arch. This requires a combination of tendon re-routing procedures, ligament repairs, and bone cutting or fusion procedures.

Fallen arches, also know as having flat feet, or pes planus, refers to the collapsing of the foot?s arch so that it is no longer curved properly or adequately supportive. The condition can cause foot pain, fatigue and affect gait, which can create strain on the knees, ankles legs and hips. Fallen arches can occur naturally from birth, or can be attributed to the rolling in of the foot and ankle while running (overpronation).
Causes
Genetic predisposition. Faulty foot mechanics, e.g. excessive pronation. Abnormal bony architecture. Laxity of ligaments. Neuro-muscular disease. Trauma to the leg muscles or major tendons. Inflammatory diseases of the joints e.g. Rheumatoid arthritis. Surgical procedures on the leg and ankle. Limb length inequality. Tight Achilles tendon.
Symptoms
Flat feet can cause a myriad of symptoms, from experiencing pain in the foot, heels, arch, calves, the shin, the knee, the hip and into the lower back due to overworking of the hip flexors or they may find it hard to stand on tip toes.
Diagnosis
People who have flat feet without signs or symptoms that bother them do not generally have to see a doctor or podiatrist about them. However, if any of the following occur, you should see your GP or a podiatrist. The fallen arches (flat feet) have developed recently. You experience pain in your feet, ankles or lower limbs. Your unpleasant symptoms do not improve with supportive, well-fitted shoes. Either or both feet are becoming flatter. Your feet feel rigid (stiff). Your feet feel heavy and unwieldy. Most qualified health care professionals can diagnose flat feet just by watching the patient stand, walk and examining his/her feet. A doctor will also look at the patient's medical history. The feet will be observed from the front and back. The patient may be asked to stand on tip-toe while the doctor examines the shape and functioning of each foot. In some cases the physician may order an X-ray, CT (computed tomography) scan, or MRI (magnetic resonance imaging) scan.
What is PES Planovalgus deformity?
Non Surgical Treatment
If you have flat feet and foot pain, especially if one foot is flatter than the other, you should have an evaluation by an orthopedic surgeon . You may have a problem with the posterior tibial tendon , the main tendon that supports the arch. Factors that can contribute to this problem are obesity, diabetes , high blood pressure , certain types of arthritis and athletic overuse. In some cases a shoe insert/orthotic can be used to alleviate the symptoms of flat feet.
Surgical Treatment

Rarely does the physician use surgery to correct a foot that is congenitally flat, which typically does not cause pain. If the patient has a fallen arch that is painful, though, the foot and ankle physicians at Midwest Orthopaedics at Rush may perform surgery to reconstruct the tendon and "lift up" the fallen arch. This requires a combination of tendon re-routing procedures, ligament repairs, and bone cutting or fusion procedures.




 Morton's neuroma is named after Dr Morton who first described this condition in 1876. It is sometimes called Morton's metatarsalgia or interdigital neuroma. It is a condition that affects one of the common plantar digital nerves that run between the long bones (metatarsals) in the foot. It most commonly affects the nerve between the third and fourth metatarsal bones, causing pain and numbness in the third and fourth toes. It can also affect the nerve between the second and third metatarsal bones, causing symptoms in the second and third toes. Morton's neuroma rarely affects the nerve between the first and second, or between the fourth and fifth, metatarsal bones. It tends to affect only one foot. It is rare to get two neuromas at the same time in the same foot.
Morton's neuroma is named after Dr Morton who first described this condition in 1876. It is sometimes called Morton's metatarsalgia or interdigital neuroma. It is a condition that affects one of the common plantar digital nerves that run between the long bones (metatarsals) in the foot. It most commonly affects the nerve between the third and fourth metatarsal bones, causing pain and numbness in the third and fourth toes. It can also affect the nerve between the second and third metatarsal bones, causing symptoms in the second and third toes. Morton's neuroma rarely affects the nerve between the first and second, or between the fourth and fifth, metatarsal bones. It tends to affect only one foot. It is rare to get two neuromas at the same time in the same foot.


 Overview
Overview Symptoms
Symptoms Overview
Overview
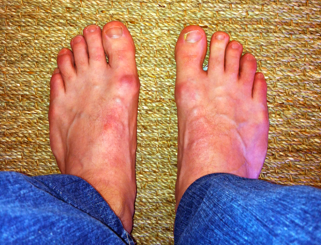 Hallux valgus, often referred to as "a bunion," is a deformity of the big toe. The toe tilts over towards the smaller toes and a bony lump appears on the inside of the foot. (A bony lump on the top of the big toe joint is usually due to a different condition, called hallux rigidus.) Sometimes a soft fluid swelling develops over the bony lump. The bony lump is the end of the "knuckle-bone" of the big toe (the first metatarsal bone) which becomes exposed as the toe tilts out of place.
Hallux valgus, often referred to as "a bunion," is a deformity of the big toe. The toe tilts over towards the smaller toes and a bony lump appears on the inside of the foot. (A bony lump on the top of the big toe joint is usually due to a different condition, called hallux rigidus.) Sometimes a soft fluid swelling develops over the bony lump. The bony lump is the end of the "knuckle-bone" of the big toe (the first metatarsal bone) which becomes exposed as the toe tilts out of place.